Login
Welcome back! Please enter your details.
or
Don't have an account? Register here
Create Account
Join MedMentorEdu and start your medical journey.
or
Already have an account? Login here
Enhance your knowledge with our comprehensive guide and curated study materials.
Asteatotic eczema is a type of eczema that develops on very dry skin, typically affecting the elderly.
Synonyms:
Eczéma craquelé
Winter eczema
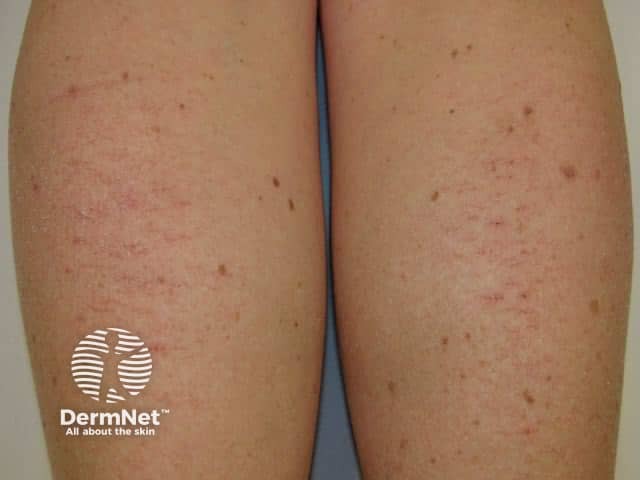
Characterized by a ‘crazy-paving’ pattern on the skin, especially the legs.
A study in Japanese elderly care home residents found a prevalence of:
16.4% in rehabilitation patients
41.2% in long-term residents
Primarily affects older adults
Incidence increases with age
Insufficient evidence on gender predisposition
Affects all ethnic groups
Hypothyroidism (myxoedema) may present with asteatotic eczema
Zinc deficiency is also a potential cause
Naturally dry skin or a lifelong tendency to chapping
Age-related reduction in skin lipids due to illness, malnutrition, or hormonal decline
Increased transpiration relative to environmental moisture levels
Loss of the epidermal water barrier in the stratum corneum
Frequent exposure to degreasing agents (cleansers, soaps, solvents)
Low environmental humidity, especially in winter months and with central heating
Repeated minor skin trauma leading to inflammation and disruption of lipid balance
Diuretics
Cimetidine
Cold, dry winds
Indoor heating
Excessive bathing
Intense irritation that worsens with temperature changes, particularly at night
Itching and burning sensations
Dry, scaly, cracked skin with a superficial crisscross pattern
‘Parchment pulps’ – dry, cracked fingertips that retain indentations after pressure
Crazy-paving pattern (Eczéma craquelé) – deep skin fissures, particularly on the legs
In severe cases:
Fissures may bleed
Skin becomes erythematous with raised edges
Legs, arms, and hands are most commonly affected
Symptoms worsen in winter and improve in summer
Chronic scratching can lead to more widespread eczema
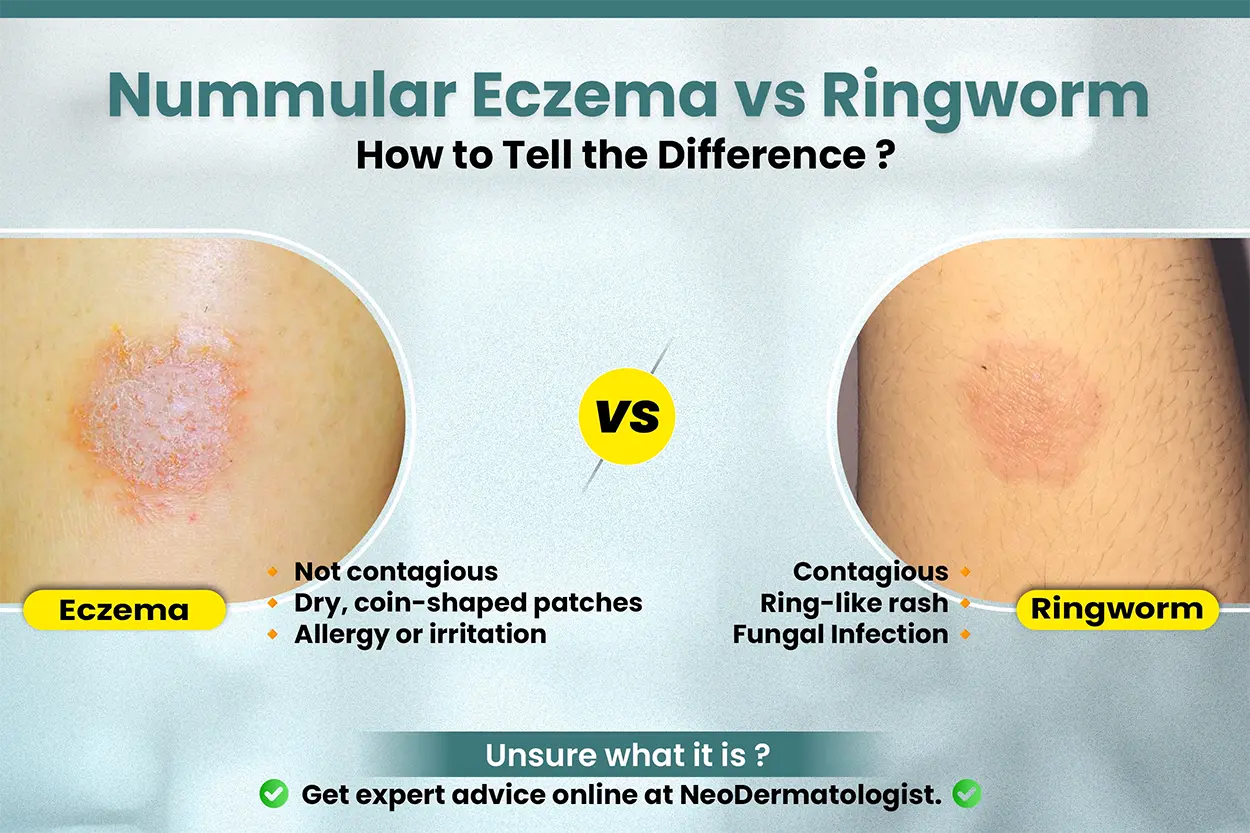
Nummular dermatitis:
Coin-shaped eczematous plaques
Psoriasis:
Well-demarcated plaques
Thick silvery scales
Ichthyosis:
Generalized scaling
Minimal/no inflammation
Cutaneous lymphoma:
Consider in:
Extensive
Atypical
Treatment-resistant cases
Tinea corporis:
Annular lesions
Central clearing
4
Secondary infections:
Due to impaired skin barrier
Nummular eczema:
May develop on background of asteatotic eczema
Chronic persistence:
Can lead to:
Permanent skin changes if untreated
Based on:
History
Physical examination
Not routinely required
Indicated only in:
Generalized disease
Suspected systemic causes
Consider in:
Atypical cases
Treatment-resistant lesions
Humidify indoor air
Avoid:
Sudden temperature changes
Dry environments
Reduce exposure to:
Harsh soaps
Detergents
Avoid:
Hot baths → use lukewarm water
Apply:
Emollients immediately after bathing
Avoid:
Wool clothing (irritant)
Cornerstone of therapy
Lanolin-based creams
Paraffin-based creams
Urea-based creams (improve hydration)
Reduce:
Skin irritation
Mild potency
Used for:
Inflamed areas


4
Topical calcineurin inhibitors:
Tacrolimus
Pimecrolimus
Useful as:
Steroid-sparing agents
Phototherapy:
Narrowband UVB
PUVA
Systemic immunosuppressants:
Methotrexate
Cyclosporine
Oral corticosteroids:
Short courses for severe flares
Antibiotics:
Oxytetracycline
Clarithromycin
(for secondary infection)
Coal tar:
For chronic lesions
Wet dressings:
For:
Severely cracked skin
Chronic, relapsing condition
Worse in:
Winter
Improves in:
Summer
Untreated:
May become persistent/permanent
Early treatment:
Excellent improvement with hydration therapy
Asteatotic eczema is a common condition in elderly individuals with dry skin
Core management:
Barrier repair + hydration
Prevention:
Humidity control + regular emollients
✔ Early intervention is key to prevent chronicity and complications
Get the full PDF version of this chapter.