Login
Welcome back! Please enter your details.
or
Don't have an account? Register here
Create Account
Join MedMentorEdu and start your medical journey.
or
Already have an account? Login here
Enhance your knowledge with our comprehensive guide and curated study materials.

4
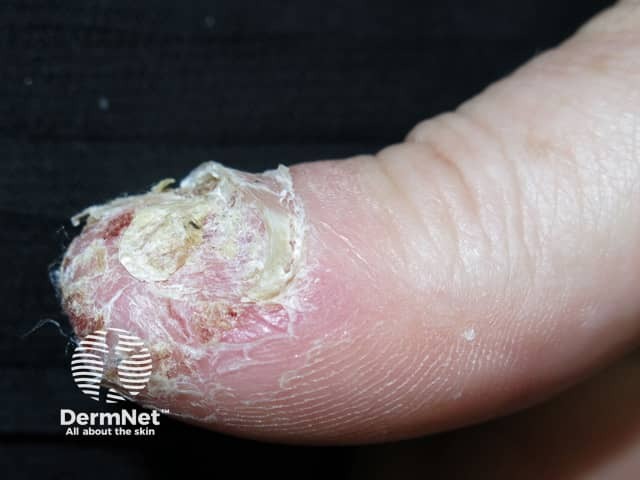
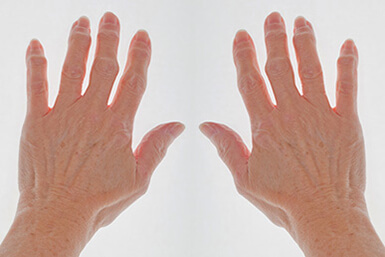
A rare, chronic, and sterile pustular skin disorder affecting the fingers or toes.
Often involves the nail beds, leading to deformity or destruction of the distal phalanx.
Considered a localized variant of pustular psoriasis with unique features and progression.
Rarity: Uncommon disorder, mostly sporadic cases.
Age of Onset: Can occur at any age, more common in adults and elderly.
Gender Predominance: Slight female predominance.
Triggering Factors:
Minor trauma, infections, external irritants.
May be exacerbated by systemic corticosteroids.
Primary Lesion:
Erythematous, scaly patches or plaques.
Sterile pustules at tips of fingers (rarely toes).
Commonly involves one or two digits, especially the thumb.
Symptoms:
Pustules rupture → crusts or erosions.
Pain, tenderness, discomfort.
4
Nail Involvement:
Nail folds, bed, matrix involvement →
Nail dystrophy
Complete loss of nail plates (onycholysis)
Chronic disease → permanent nail destruction
Bone and Joint Changes:
Osteolysis (loss of distal phalanx)
Joint stiffness or deformity (resembles psoriatic arthritis)
Spread:
Proximal extension along digit
May involve multiple digits
Generalization:
Can progress to generalized pustular psoriasis (life-threatening)
Localized Pattern: Limited to one/few digits, chronic course.
Diffuse Pattern: Progressive spread with generalized pustulation.


4
Autoimmune Nature:
Dysregulation of innate immunity
Neutrophil activation
Elevated IL-36 cytokines
Genetic Associations:
Mutations in IL36RN
Mutations in AP1S3
Triggers:
Trauma, stress, infections, irritants
4
Subcorneal neutrophilic pustules (hallmark).
Spongiform pustules, parakeratosis, epidermal thinning.
Chronic cases:
Epidermal atrophy
Fibrosis
Dermal inflammation
Key feature: Absence of infectious agents in pustules.
Clinical diagnosis based on characteristic lesions.
Laboratory tests:
Rule out bacterial/fungal infections (sterile pustules).
Genetic testing (IL36RN, AP1S3).
Imaging:
X-ray → detect osteolysis or deformities.
Histology:
Confirms neutrophilic pustules.
Infectious:
Herpetic whitlow
Candidiasis
Inflammatory:
Psoriatic arthritis
Onychomycosis
Parakeratosis pustulosa
Traumatic:
Traumatic onycholysis
Contact dermatitis
Chronic and relapsing.
Persists for months to years.
Complications:
Nail destruction
Severe deformity and disability
Spontaneous remission: Rare

4
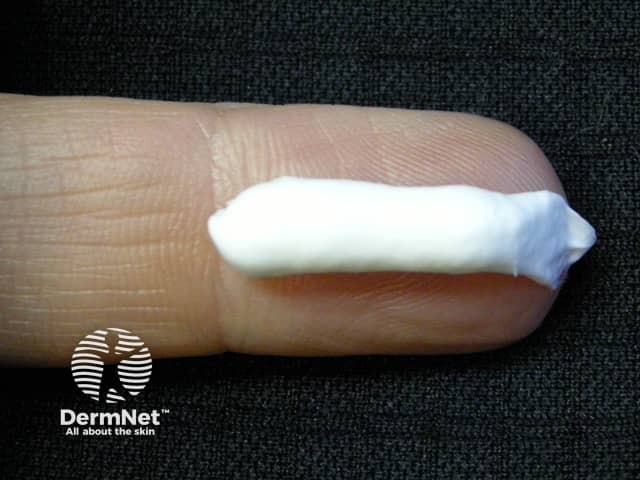
Topical corticosteroids (with occlusion).
Vitamin D analogues (calcipotriol).
Topical tacrolimus.
5
First-line:
Acitretin (0.3–0.5 mg/kg/day)
Methotrexate
Ciclosporin
Second-line:
Biologics:
TNF-α inhibitors (Infliximab, Adalimumab)
IL-17 inhibitors (Secukinumab)
IL-23 inhibitors (Ustekinumab)
IL-1 blockade: Anakinra
Acitretin + PUVA
Methotrexate + biologics
Protect digits from trauma.
Treat secondary infections if present.
Localized ACH:
Treatable but relapsing
Functional impairment possible
Generalized ACH:
Requires aggressive therapy
High morbidity
4
Early diagnosis prevents nail loss and bone deformities.
IL36RN mutation testing helps guide biologic therapy.
Long-term remission often requires multimodal treatmen
Get the full PDF version of this chapter.