Login
Welcome back! Please enter your details.
or
Don't have an account? Register here
Create Account
Join MedMentorEdu and start your medical journey.
or
Already have an account? Login here
Enhance your knowledge with our comprehensive guide and curated study materials.
• Definition
• Micturition refers to the process of emptying urine from the urinary bladder through the urethra.
• Physiological nature
• It is a reflex process controlled by the spinal cord, but also influenced by higher brain centers.
• Functions of urinary bladder
• Temporary storage of urine
• Periodic elimination of urine.
• Control mechanisms involved
• Nervous control
• Muscular contraction of bladder wall
• Relaxation of urethral sphincters.
The act of urination may feel simple, but physiologically it is a finely tuned collaboration between smooth muscle, spinal reflexes, and conscious brain control.
• Nature of organ
• The urinary bladder is a hollow muscular organ located in the pelvic cavity.
• Main parts
• Apex
• Body
• Fundus (base)
• Neck.
• Wall structure
• Mucous membrane
• Muscular layer (detrusor muscle)
• Outer connective tissue layer.
• Important region
• Trigone – triangular area between the openings of ureters and urethra.
• Function of detrusor muscle
• Responsible for contraction of bladder during micturition.
The bladder wall is highly elastic. It can stretch remarkably, storing 400–600 mL of urine without a major rise in pressure.



• Continuous urine flow
• Urine produced by kidneys enters the bladder through ureters.
• Detrusor muscle during filling
• Remains relaxed allowing bladder expansion.
• Internal sphincter
• Remains contracted preventing urine leakage.
• Nervous control
• Sympathetic nerves help maintain bladder relaxation during storage phase.
• Bladder capacity
• Normally stores about 400–500 mL of urine.
• Sensation of fullness
• Stretch receptors in bladder wall send signals to spinal cord and brain.
The bladder behaves like a biological reservoir with elastic walls—it fills quietly for long periods before the nervous system decides it is time to empty.
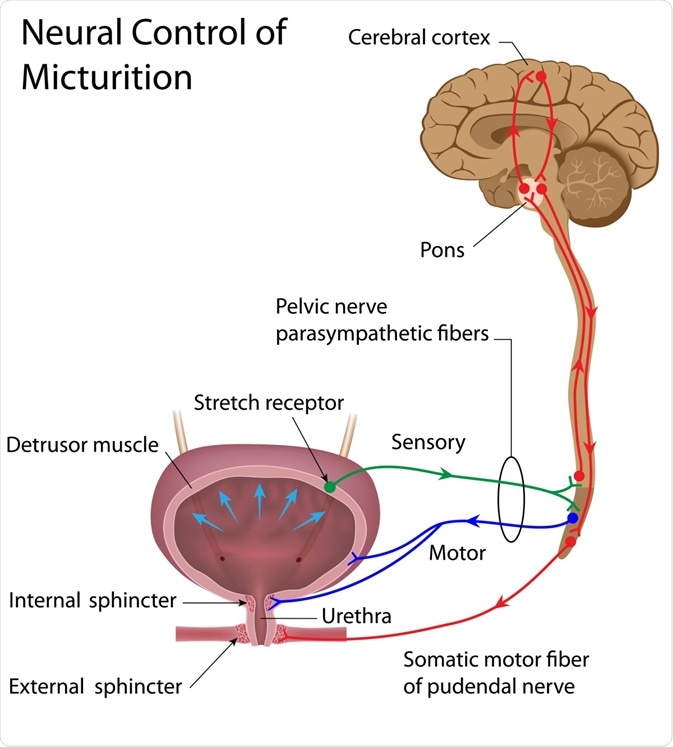
• Trigger
• When bladder fills to about 300–400 mL, stretch receptors are activated.
• Reflex pathway
• Signals travel through pelvic nerves to the spinal cord.
• Parasympathetic activation
• Causes contraction of detrusor muscle.
• Sphincter relaxation
• Internal urethral sphincter relaxes.
• Voluntary control
• External urethral sphincter controlled by somatic nerves (pudendal nerve).
• Urine expulsion
• Coordinated contraction of bladder and relaxation of sphincters results in urination.
In physiological terms, micturition is a spinal reflex that learned to cooperate with consciousness. Infants rely entirely on reflex control, but the developing brain gradually gains the ability to delay or initiate the process.

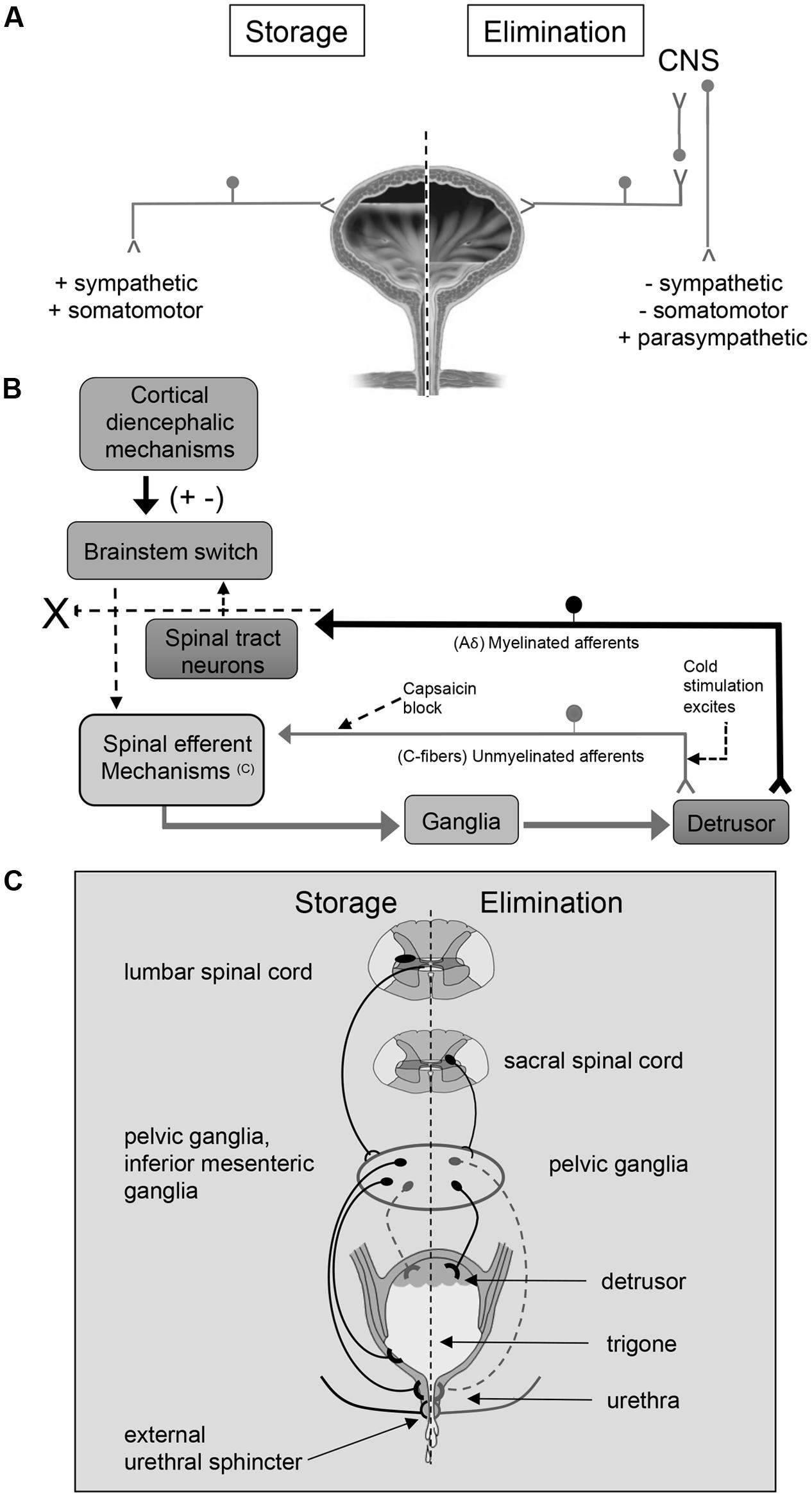
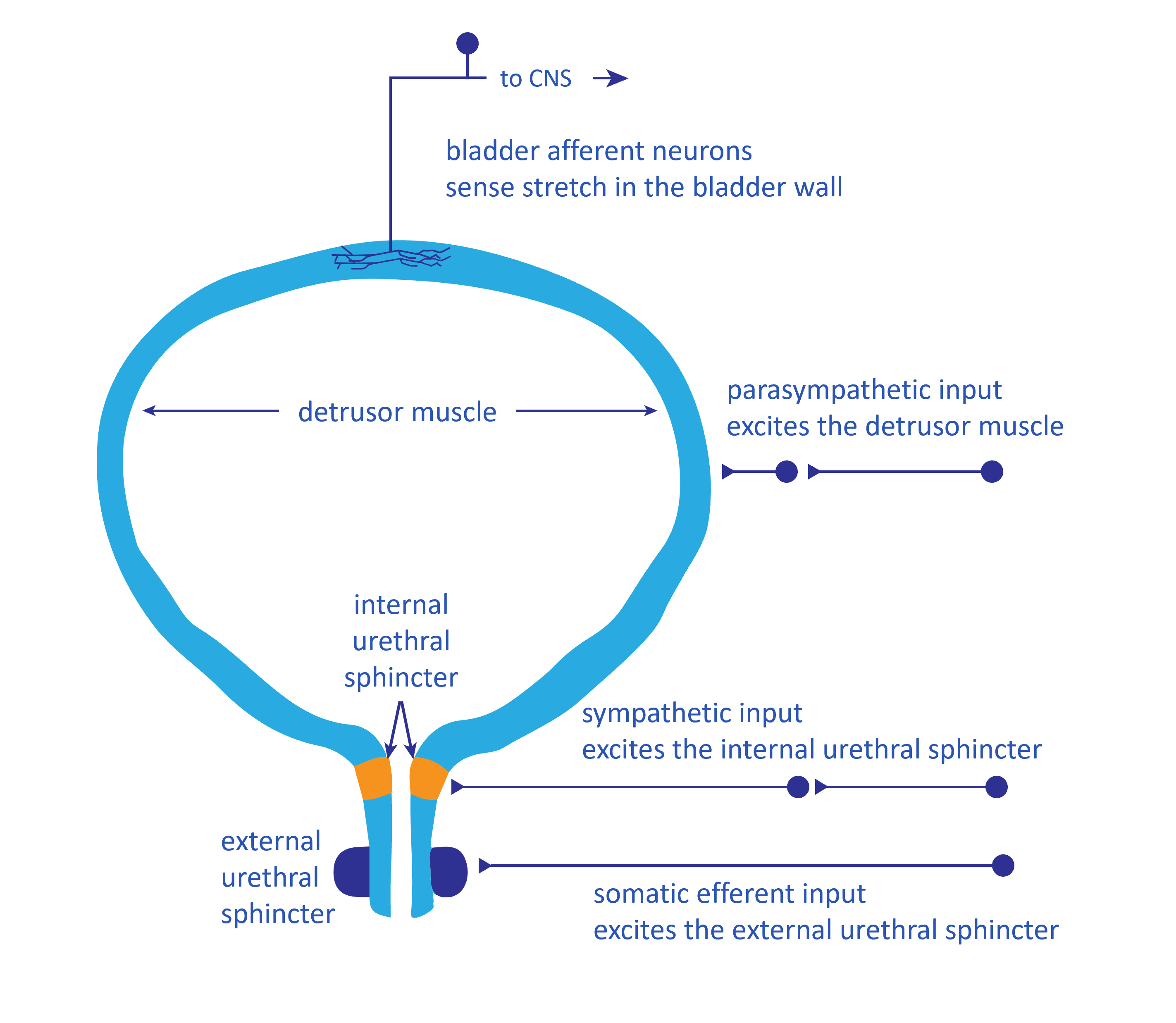

• Definition
• Micturition reflex is a spinal reflex responsible for emptying the urinary bladder.
• Stimulus
• Stretching of the bladder wall due to accumulation of urine.
• Receptors involved
• Stretch receptors located in the bladder wall.
• Afferent pathway
• Impulses travel through pelvic nerves to the sacral spinal cord (S2–S4).
• Efferent pathway
• Parasympathetic fibers return through pelvic nerves.
• Response
• Contraction of detrusor muscle
• Relaxation of internal urethral sphincter.
• Nature of reflex
• It is automatic but can be voluntarily controlled by higher brain centers.
The reflex behaves like a rhythmic cycle—stretch → reflex contraction → partial emptying—until voluntary control either permits or suppresses the act of urination.

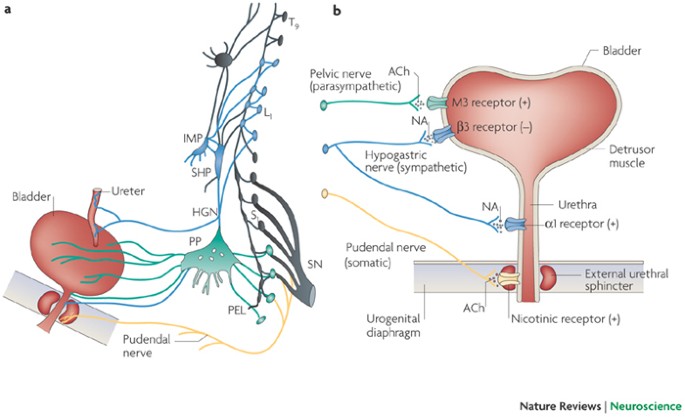
• Micturition is regulated not only by spinal reflexes but also by higher nervous centers.
• These centers help in coordination, voluntary control and inhibition of urination.
• Main centres involved
• Cortical centre
• Hypothalamic centre
• Brain stem centre.
These higher centres transform the primitive spinal reflex into a behavior under conscious control, allowing humans to decide the socially appropriate moment to void.


• Location
• Located in the cerebral cortex, particularly in the frontal lobe.
• Function
• Provides voluntary control over micturition.
• Mechanism
• Can either facilitate or inhibit the spinal micturition reflex.
• Physiological importance
• Enables conscious control of urination.
• Clinical relevance
• Damage to cortical areas may lead to loss of voluntary bladder control.
The cortex acts like the executive decision-maker, deciding whether the reflex should proceed or be temporarily suppressed.

• Location
• Situated in the hypothalamus of the brain.
• Function
• Integrates autonomic regulation of bladder activity.
• Role
• Coordinates bladder function with emotional and autonomic responses.
• Physiological significance
• Helps maintain appropriate bladder control during various physiological states.
The hypothalamus acts like a physiological coordinator, linking bladder activity with the body’s internal state—stress, hydration, and autonomic balance.

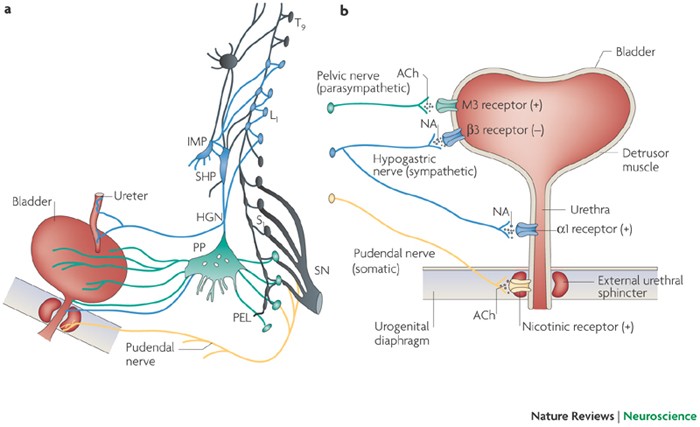
• Location
• Located in the pons of the brain stem.
• Name
• Known as the pontine micturition centre (PMC).
• Function
• Coordinates contraction of bladder and relaxation of urethral sphincters.
• Role in urination
• Ensures smooth and coordinated voiding of urine.
• Physiological importance
• Prevents simultaneous contraction of bladder and sphincters.
This small cluster of neurons in the pons functions like a biological conductor, synchronizing bladder contraction and sphincter relaxation so that urine flows efficiently rather than chaotically.
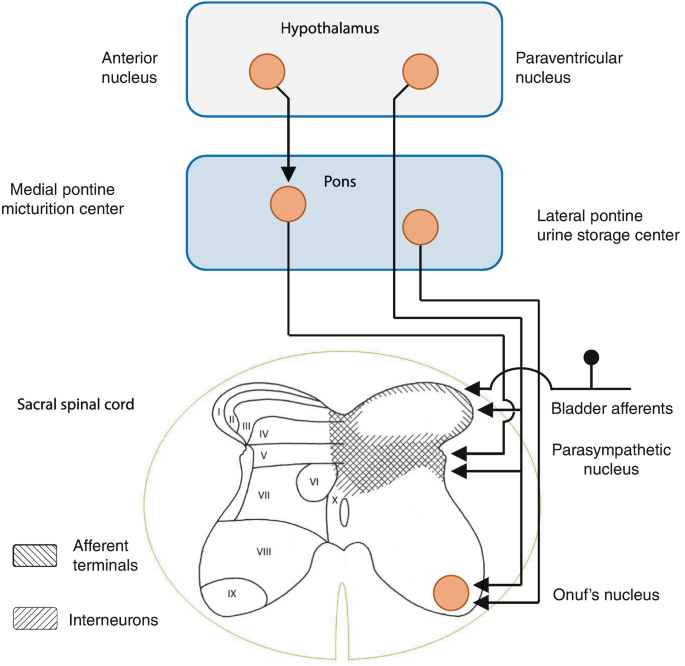



• Location
• Spinal centres for micturition are located in the sacral segments of the spinal cord (S2–S4).
• Function
• These centres control the basic micturition reflex.
• Afferent impulses
• Stretch receptors in bladder wall send signals to the sacral spinal cord via pelvic nerves.
• Efferent impulses
• Parasympathetic fibers return from spinal cord to bladder.
• Response produced
• Contraction of detrusor muscle
• Relaxation of internal urethral sphincter.
• Physiological importance
• Responsible for automatic bladder emptying in infants and spinal animals.
Before the brain’s higher centers develop control, the spinal cord alone manages urination through this primitive reflex circuit.


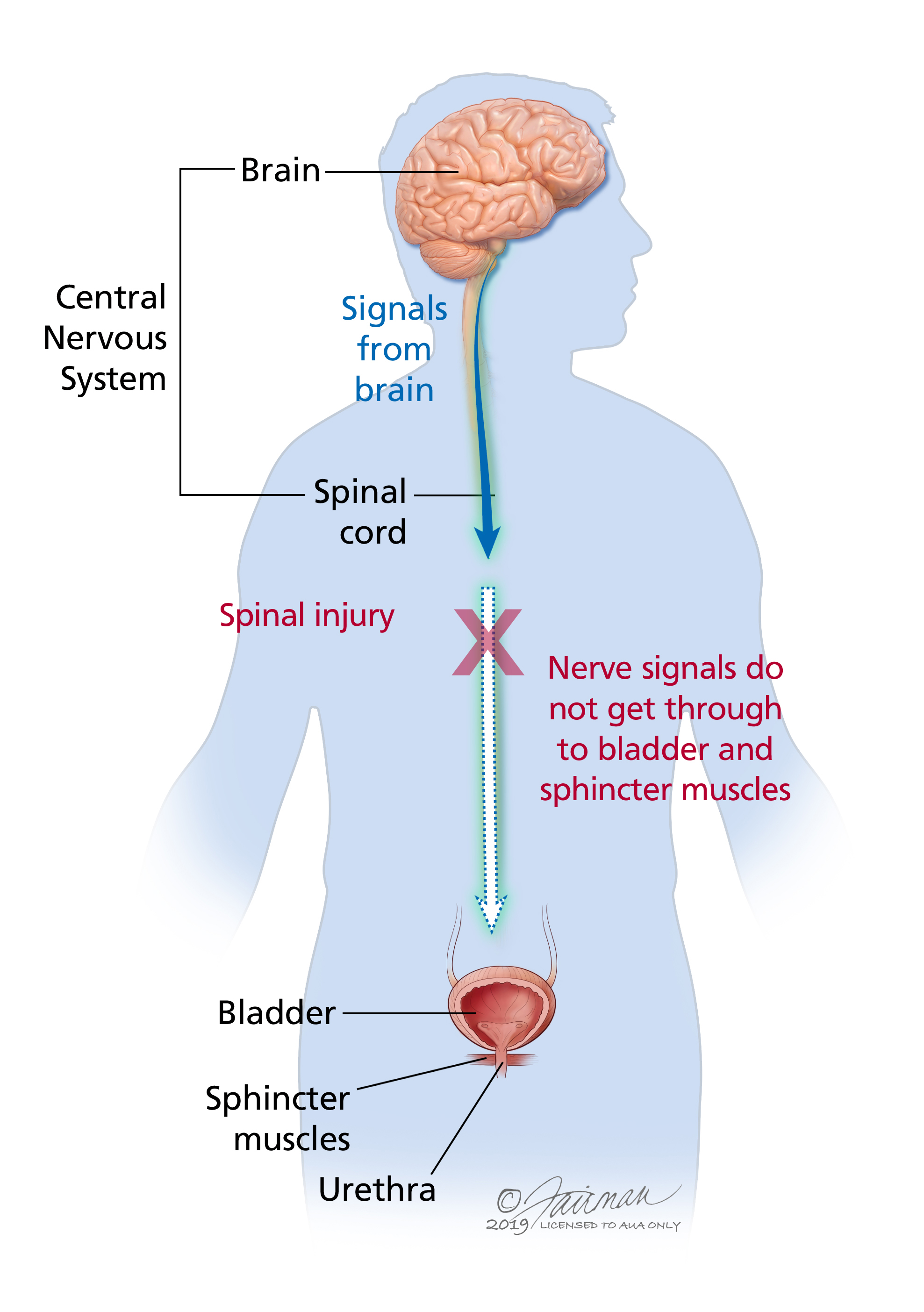
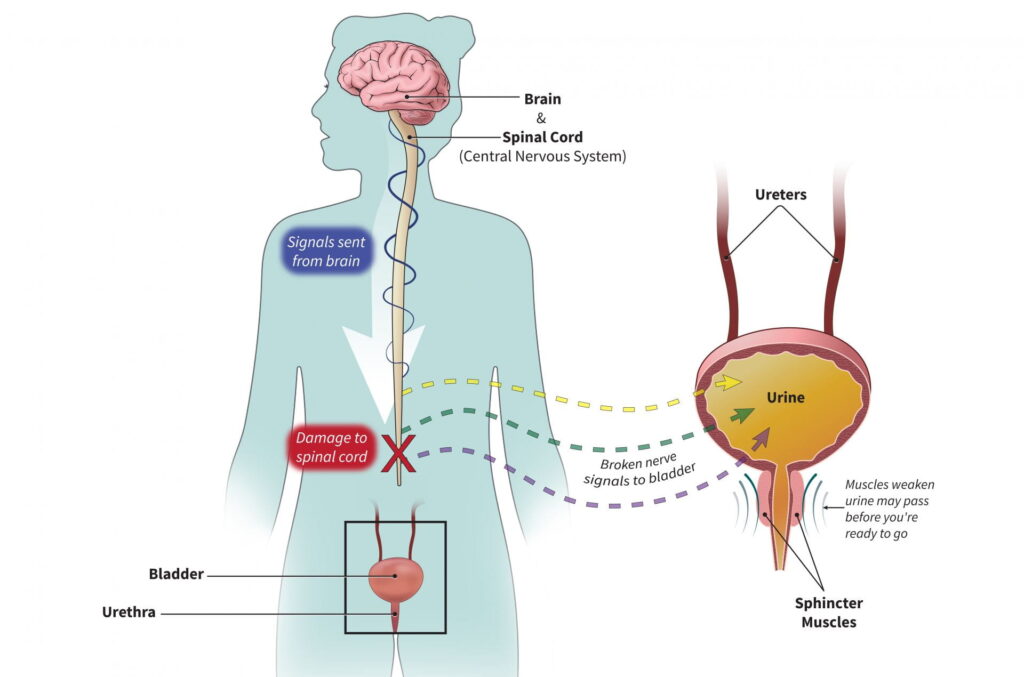
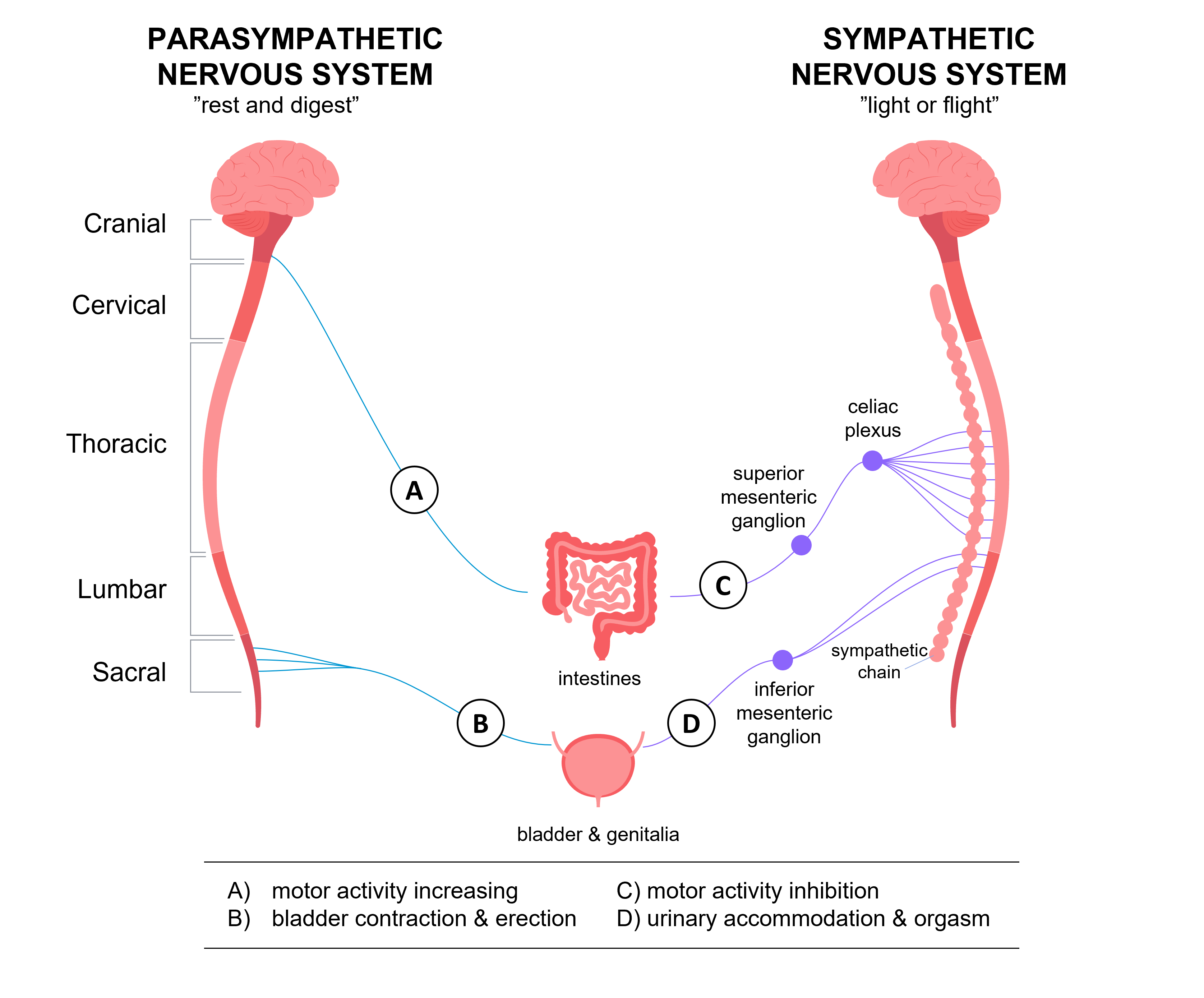
• Autonomic nerves involved
• Parasympathetic nerves (pelvic nerves)
• Sympathetic nerves.
• Effect of damage
• Loss of normal autonomic regulation of bladder function.
• Physiological consequence
• Bladder may become distended due to inability to empty properly.
• Urinary problems produced
• Urinary retention
• Overflow incontinence.
• Clinical significance
• Seen in spinal cord injury or neuropathies affecting pelvic nerves.
Damage to these nerves disrupts the delicate balance between storage and emptying phases of the bladder.




• Efferent nerves involved
• Parasympathetic fibers supplying the detrusor muscle.
• Effect of lesion
• Detrusor muscle cannot contract effectively.
• Result
• Bladder becomes large and flaccid.
• Urinary consequence
• Urine accumulates leading to retention of urine.
• Secondary effect
• Gradual overflow incontinence may occur.
Physiologically this produces a flaccid or atonic bladder—a reservoir that keeps filling but cannot generate the muscular force needed to empty itself.



• Origin
• Parasympathetic fibres arise from sacral segments of spinal cord (S2–S4).
• Pathway
• Travel through pelvic nerves to the urinary bladder.
• Function
• Stimulate contraction of the detrusor muscle.
• Effect on sphincters
• Promote relaxation of the internal urethral sphincter.
• Role in micturition
• Responsible for emptying of the urinary bladder.
These nerves are essentially the “voiding pathway” of the bladder—when activated, they convert the bladder from a storage organ into an expelling pump.


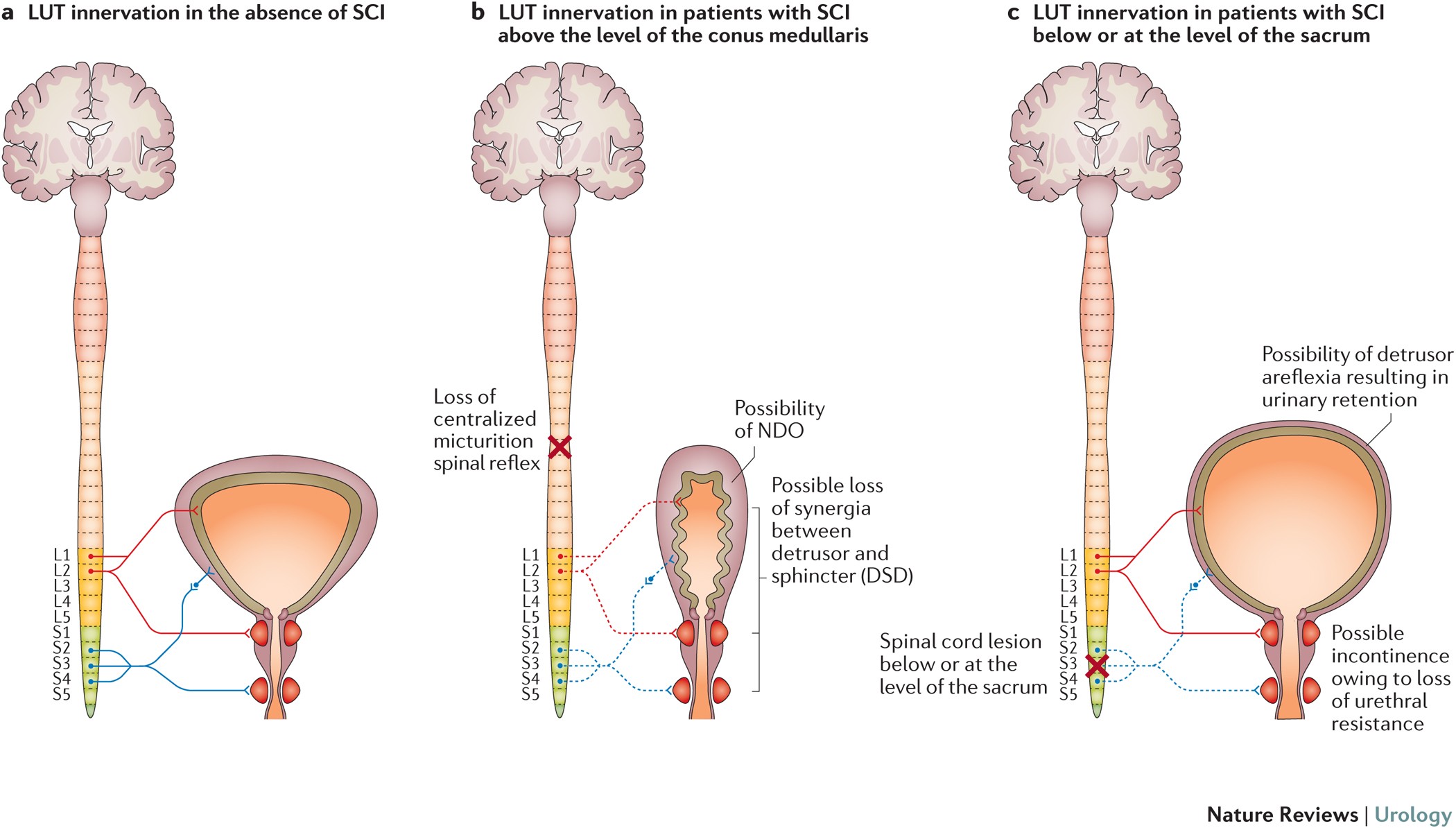
• Initial stage (spinal shock)
• Immediately after spinal cord transection, micturition reflex is abolished.
• Bladder condition
• Bladder becomes distended and urine accumulates.
• Urinary outcome
• Urinary retention occurs during early phase.
• Later stage
• Spinal reflex gradually returns.
• Result
• Bladder empties automatically without voluntary control.
• Condition produced
• Known as automatic bladder.
This phenomenon illustrates a curious principle in neurophysiology: when higher control is lost, primitive spinal reflexes eventually re-emerge and operate independently.
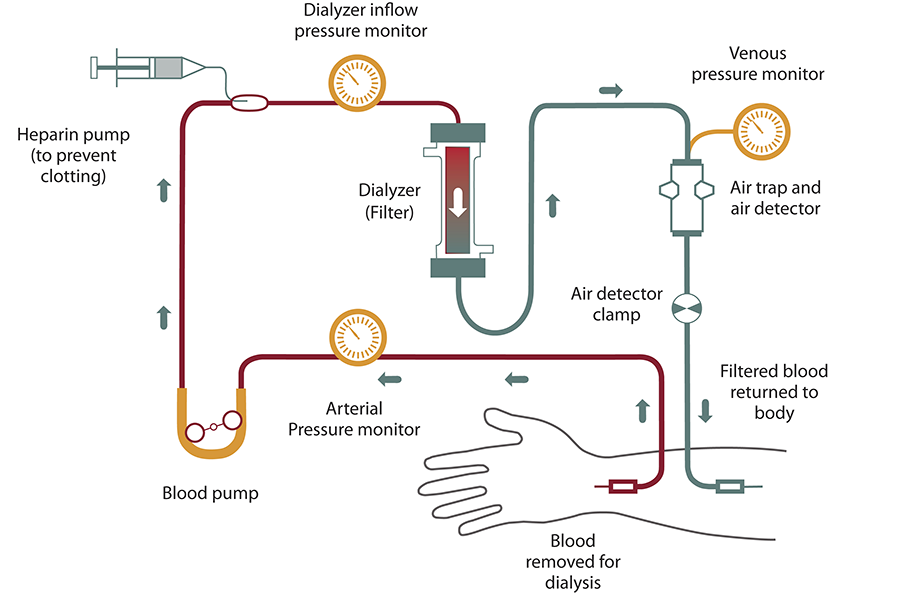
• Definition
• Artificial kidney refers to a dialysis machine used to remove waste products from blood when kidneys fail.
• Principle
• Based on diffusion and ultrafiltration through a semipermeable membrane.
• Process
• Blood flows through a dialyzer containing dialysis fluid.
• Substances removed
• Urea
• Creatinine
• Excess electrolytes
• Excess water.
• Clinical use
• Used in acute renal failure and chronic kidney disease.
• Purpose
• Maintains chemical balance of blood until kidney function recovers or transplantation is performed.
Dialysis machines are a fascinating example of physiology translated into engineering. They replicate one of the kidney’s core tricks—separating useful molecules from wastes using selective membranes and concentration gradients.
Get the full PDF version of this chapter.