Login
Welcome back! Please enter your details.
or
Don't have an account? Register here
Create Account
Join MedMentorEdu and start your medical journey.
or
Already have an account? Login here
Enhance your knowledge with our comprehensive guide and curated study materials.
• System responsible for removal of metabolic wastes
• The excretory system eliminates waste products formed during metabolism.
• Maintenance of internal environment
• It plays a major role in maintaining water balance, electrolyte balance and acid–base balance.
• Major organs of excretory system
• Kidneys
• Ureters
• Urinary bladder
• Urethra.
• Formation and elimination of urine
• Kidneys filter blood to form urine containing metabolic waste products and excess substances.
• Regulation of body fluids
• The system helps regulate blood volume, osmotic balance and blood pressure.
From a physiological viewpoint, the excretory system is the body’s chemical purification plant, continuously filtering the blood to maintain internal stability.
• Paired excretory organs
• Kidneys are two bean-shaped organs located in the posterior abdominal wall.
• Position in body
• They lie on either side of the vertebral column in the lumbar region.
• Main functions
• Formation of urine
• Excretion of metabolic waste products
• Regulation of water and electrolyte balance
• Maintenance of acid–base balance.
• Structural unit of kidney
• The functional unit of the kidney is the nephron, which carries out filtration and urine formation.
• Blood supply
• Kidneys receive blood through the renal arteries and drain through renal veins.
Each kidney contains millions of nephrons, tiny filtration units that together perform the enormous task of cleansing the body’s circulating blood.
• Shape and size
• Kidneys are bean-shaped organs measuring about 10–12 cm in length.
• External surface
• Each kidney has a smooth convex lateral surface and a concave medial border.
• Renal hilum
• The medial border contains a hilum through which blood vessels, nerves and ureter pass.
• Internal structure
• The kidney consists of outer cortex and inner medulla.
• Renal pyramids
• The medulla contains renal pyramids whose apices open into minor calyces.
• Renal pelvis formation
• Minor calyces join to form major calyces, which unite to form the renal pelvis leading to the ureter.
The kidney’s architecture reflects its function: blood arrives through the hilum, is processed through millions of microscopic filtration units, and the resulting filtrate ultimately leaves the organ as urine through the ureter.
4
• Structural and functional unit of kidney
• The nephron is the basic unit responsible for formation of urine.
• Number of nephrons
• Each kidney contains approximately one million nephrons.
• Major components of nephron
• Renal corpuscle
• Renal tubule.
• Renal corpuscle
• Consists of glomerulus and Bowman’s capsule, where filtration of blood occurs.
• Renal tubule parts
• Proximal convoluted tubule
• Loop of Henle
• Distal convoluted tubule.
• Functions of nephron
• Filtration of blood
• Reabsorption of useful substances
• Secretion of certain substances into the filtrate
• Formation of urine.
The nephron is essentially a microscopic chemical processing unit, filtering blood plasma and selectively reclaiming substances the body still needs.
• Tubular system involved in urine formation
• Uriniferous tubules are the microscopic tubular structures responsible for formation and transport of urine.
• Components of uriniferous tubule
• Each uriniferous tubule consists of:
• Nephron
• Collecting tubule (collecting duct).
• Function of nephron portion
• The nephron carries out filtration, reabsorption and secretion.
• Function of collecting tubules
• Collecting ducts receive urine from multiple nephrons and transport it toward renal pelvis.
• Pathway of urine flow
• Urine formed in nephrons passes through collecting ducts, renal calyces and renal pelvis before entering the ureter.
Physiologically, the uriniferous tubules form an intricate drainage network, collecting filtrate from millions of nephrons and channeling it toward the urinary tract.

4
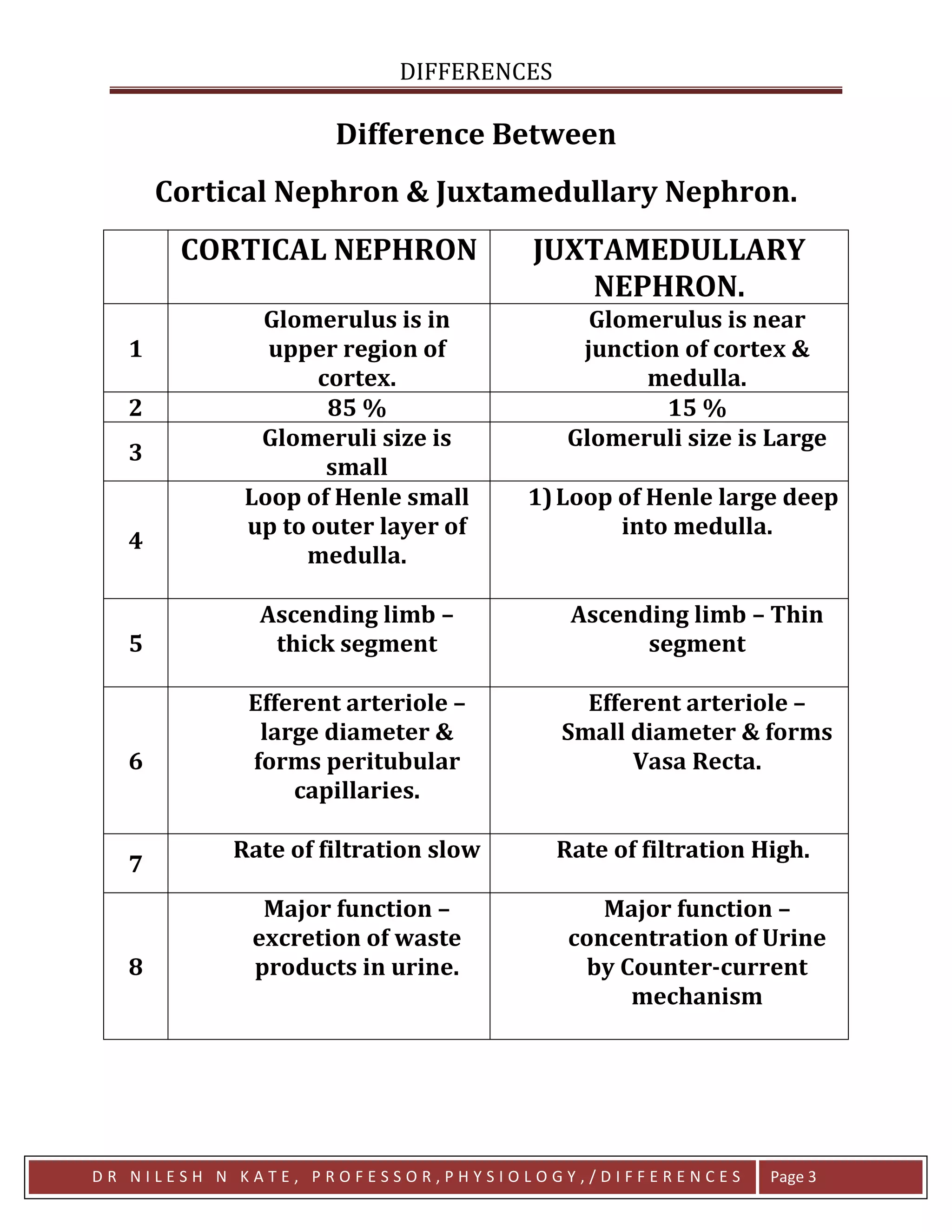
• Two main types of nephrons are present in the kidney
• Cortical nephrons
• Located mainly in the outer cortex of the kidney.
• Have short loops of Henle.
• Represent the majority of nephrons (about 85%).
• Mainly involved in filtration and reabsorption.
• Juxtamedullary nephrons
• Located near the junction of cortex and medulla.
• Possess long loops of Henle extending deep into the medulla.
• Important for concentration of urine.
The kidney cleverly uses two nephron designs. Cortical nephrons handle most routine filtration, while juxtamedullary nephrons—with their long loops—act as the precision machinery that allows the body to concentrate urine and conserve water.
4
• Tubular portion of the nephron
• Renal tubules are the elongated tubular structures of the nephron where filtration products are modified to form urine.
• Continuation from Bowman’s capsule
• The renal tubule begins at Bowman’s capsule and ends by joining the collecting duct.
• Major parts of renal tubule
• Proximal convoluted tubule
• Loop of Henle
• Distal convoluted tubule.
• Functions of renal tubules
• Reabsorption of useful substances
• Secretion of waste products
• Regulation of water and electrolyte balance.
• Modification of glomerular filtrate
• As filtrate passes through renal tubules, it is selectively modified to produce final urine.
The renal tubules function as a fine-tuning laboratory—after the initial filtration in the glomerulus, these tubules selectively reclaim valuable substances while leaving wastes behind.

4
• First segment of renal tubule
• The proximal convoluted tubule begins immediately after Bowman’s capsule.
• Location
• It lies in the cortex of the kidney.
• Highly coiled structure
• The tubule is extensively convoluted, increasing surface area for reabsorption.
• Presence of brush border
• The epithelial cells possess microvilli forming a brush border, which greatly increases absorptive capacity.
• Major site of reabsorption
• About 65–70% of glomerular filtrate is reabsorbed in the PCT.
• Substances reabsorbed
• Glucose
• Amino acids
• Sodium
• Bicarbonate
• Water.
• Secretion of substances
• Certain substances such as hydrogen ions, drugs and metabolic wastes may be secreted into the tubular fluid.
Physiologically, the PCT is the workhorse of the nephron. Most of the filtrate is reclaimed here, ensuring that essential molecules like glucose and amino acids are returned to the bloodstream rather than lost in urine.
• U-shaped segment of renal tubule
• The loop of Henle is the portion of the nephron that dips from the cortex into the medulla and returns back to the cortex.
• Parts of the loop
• Descending limb
• Ascending limb.
• Descending limb characteristics
• Highly permeable to water.
• Water moves out of the tubule into the surrounding medullary interstitium.
• Ascending limb characteristics
• Impermeable to water.
• Actively transports sodium and chloride ions out of the tubular fluid.
• Role in urine concentration
• The loop of Henle establishes the osmotic gradient in the renal medulla, essential for concentrating urine.
Physiologically, the loop of Henle acts like a countercurrent concentration device, generating the osmotic gradient that allows the kidney to conserve water when necessary.


• Segment following the loop of Henle
• The distal convoluted tubule begins where the ascending limb of the loop of Henle returns to the cortex.
• Location
• It lies in the renal cortex.
• Less convoluted than PCT
• The DCT has fewer microvilli and a smaller diameter compared with the PCT.
• Selective reabsorption
• Reabsorbs sodium, chloride and water under hormonal control.
• Hormonal regulation
• Aldosterone increases sodium reabsorption and potassium secretion.
• Antidiuretic hormone (ADH) influences water reabsorption.
• Role in electrolyte balance
• Helps maintain acid–base balance and electrolyte homeostasis.
The DCT functions like a fine adjustment segment, where hormones precisely control electrolyte and water balance before urine is finalized.


• Terminal part of uriniferous tubule
• Collecting tubules receive filtrate from multiple distal convoluted tubules.
• Pathway through kidney
• They pass through the renal cortex and medulla toward the renal pelvis.
• Final modification of urine
• Collecting ducts determine the final concentration and volume of urine.
• Hormonal influence
• Antidiuretic hormone (ADH) increases water reabsorption from collecting ducts.
• Role in urine concentration
• Water reabsorption in the medullary collecting ducts helps produce concentrated urine when required.
The collecting tubules represent the kidney’s final decision point. Depending on the body’s hydration state, they either reclaim water or allow it to pass, ultimately determining how dilute or concentrated the urine will be.
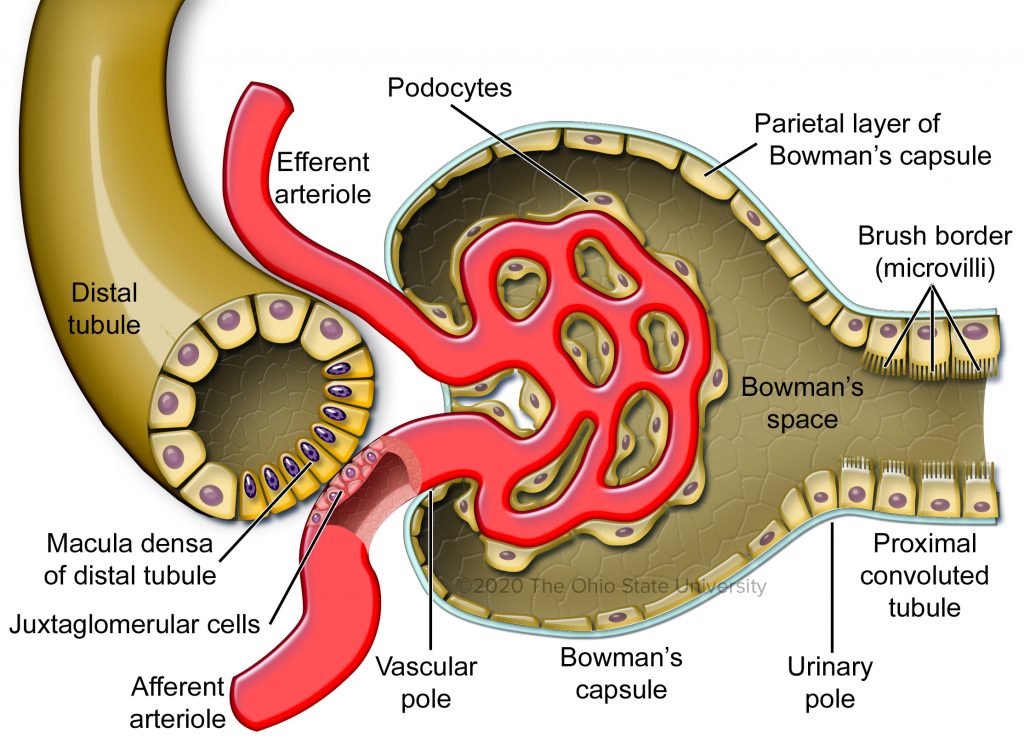


• Specialized structure in nephron
• The juxtaglomerular apparatus (JGA) is a specialized region where the distal convoluted tubule comes in close contact with the afferent arteriole of the same nephron.
• Location
• It lies near the vascular pole of the renal corpuscle.
• Components of JGA
• Macula densa
• Juxtaglomerular (JG) cells
• Lacis cells (extraglomerular mesangial cells).
• Macula densa
• A group of specialized epithelial cells in the distal convoluted tubule that detect changes in sodium chloride concentration in tubular fluid.
• Juxtaglomerular cells
• Modified smooth muscle cells of the afferent arteriole that secrete renin.
• Lacis cells
• Cells located between the afferent arteriole, efferent arteriole and distal tubule, involved in signal transmission within the JGA.
Physiologically, the JGA acts like a monitoring station of the nephron, constantly sensing changes in tubular fluid and blood flow to regulate kidney function.

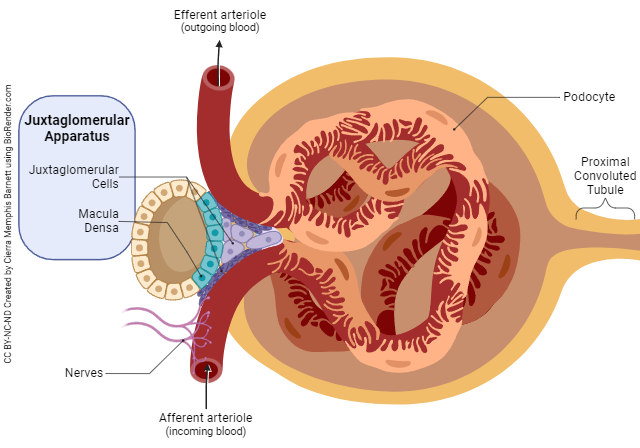

• Regulation of glomerular filtration rate (GFR)
• The JGA helps regulate filtration rate of the glomerulus.
• Control of renin secretion
• Juxtaglomerular cells release renin, an enzyme that initiates the renin–angiotensin–aldosterone system (RAAS).
• Regulation of blood pressure
• Through RAAS activation, the JGA plays a key role in maintaining systemic blood pressure.
• Monitoring sodium concentration
• The macula densa senses sodium chloride concentration in tubular fluid, adjusting renal blood flow accordingly.
• Regulation of body fluid balance
• By influencing renin secretion and filtration rate, the JGA contributes to regulation of extracellular fluid volume and electrolyte balance.
Seen through the lens of physiology, the juxtaglomerular apparatus is a tiny but powerful control center. By sensing changes in salt concentration and blood pressure, it triggers hormonal pathways that help stabilize circulation and kidney function.


• Blood supply of the kidneys
• Renal circulation refers to the flow of blood through the kidneys for filtration and urine formation.
• Entry of blood into kidney
• Blood enters the kidney through the renal artery, which arises from the abdominal aorta.
• Branching within the kidney
• The renal artery divides into segmental, interlobar, arcuate and interlobular arteries.
• Formation of glomerular capillaries
• Interlobular arteries give rise to afferent arterioles that supply the glomeruli.
• Exit of blood from glomerulus
• Blood leaves the glomerulus through the efferent arteriole.
• Formation of secondary capillary network
• Efferent arterioles form peritubular capillaries and vasa recta, which surround renal tubules.
• Venous drainage
• Blood ultimately drains into interlobular veins → arcuate veins → interlobar veins → renal vein → inferior vena cava.
Renal circulation is remarkable because the kidney receives a very large proportion of cardiac output, allowing rapid filtration of blood.

• Presence of two capillary beds
• The renal circulation contains two capillary networks in series:
• Glomerular capillaries
• Peritubular capillaries.
• Afferent and efferent arterioles
• Unlike most organs, the glomerular capillary network is situated between two arterioles rather than between an arteriole and a venule.
• High hydrostatic pressure in glomerulus
• The glomerular capillaries maintain high pressure necessary for filtration.
• Peritubular capillary function
• Peritubular capillaries facilitate reabsorption of water and solutes from renal tubules.
These features allow the kidney to perform two opposite processes simultaneously—filtration in glomeruli and reabsorption in surrounding capillaries.

• Very high renal blood flow
• Kidneys receive approximately 20–25% of cardiac output.
• Uneven distribution of blood flow
• Most renal blood flow occurs in the renal cortex, while the medulla receives relatively less blood.
• Presence of vasa recta
• In juxtamedullary nephrons, efferent arterioles form vasa recta, long straight vessels descending into the medulla.
• Role in concentration of urine
• Vasa recta help maintain the medullary osmotic gradient necessary for concentrating urine.
• Autoregulation of renal blood flow
• The kidney maintains relatively constant blood flow despite moderate changes in systemic blood pressure.
From a physiological standpoint, renal circulation is engineered for precision: high cortical blood flow ensures efficient filtration, while specialized medullary vessels preserve the osmotic gradients needed for urine concentration.
Get the full PDF version of this chapter.