Login
Welcome back! Please enter your details.
or
Don't have an account? Register here
Create Account
Join MedMentorEdu and start your medical journey.
or
Already have an account? Login here
Enhance your knowledge with our comprehensive guide and curated study materials.
• Gas exchange in lungs occurs by diffusion across the respiratory membrane
• Oxygen diffuses from alveoli into pulmonary capillary blood
• Carbon dioxide diffuses from blood into alveoli
• Efficient gas exchange requires proper matching of ventilation and perfusion
• Important for maintaining normal oxygenation of blood
• Process of diffusion in lungs
• Diffusion refers to the movement of gases from an area of higher partial pressure to lower partial pressure.
• Oxygen diffusion
• Oxygen moves from alveolar air (higher PO₂) → pulmonary capillary blood (lower PO₂).
• Carbon dioxide diffusion
• Carbon dioxide moves from blood (higher PCO₂) → alveoli (lower PCO₂).
• Respiratory membrane
• Diffusion occurs across a very thin membrane consisting of:
• Alveolar epithelium
• Interstitial space
• Capillary endothelium
• Importance of ventilation–perfusion matching
• Effective gas exchange requires adequate air reaching alveoli and adequate blood flow in pulmonary capillaries.
The respiratory membrane is astonishingly thin—about 0.5 micrometers. Nature essentially stretched a delicate film between air and blood to make diffusion extremely efficient.
• Several physical and physiological factors determine the rate of gas diffusion in lungs
4
• Partial pressure gradient
• Diffusion rate depends on the difference in partial pressure of gases between alveoli and blood.
• Surface area of respiratory membrane
• Larger surface area increases diffusion.
• Human lungs provide about 70–100 square meters of exchange surface.
• Thickness of respiratory membrane
• Diffusion decreases if membrane thickness increases.
• Seen in diseases like pulmonary fibrosis and pulmonary edema.
• Solubility of gases
• Carbon dioxide diffuses about 20 times faster than oxygen because of greater solubility.
• Molecular weight of gases
• Diffusion rate is inversely proportional to the square root of molecular weight.
This relationship is summarized by Fick’s law of diffusion, which governs how gases move across membranes.
• Measure of efficiency of lungs in transferring oxygen from alveoli to blood
• Reflects functional status of respiratory membrane

4
• Definition
• Pulmonary diffusing capacity refers to the volume of oxygen that diffuses through the respiratory membrane per minute for each mmHg difference in pressure.
• Normal diffusing capacity
• Diffusing capacity of oxygen at rest is approximately 20–25 mL/min/mmHg.
• Factors influencing diffusing capacity
• Surface area of alveoli
• Thickness of respiratory membrane
• Pulmonary blood flow
• Hemoglobin concentration
• Clinical significance
• Diffusing capacity decreases in:
• Pulmonary fibrosis
• Emphysema
• Pulmonary edema
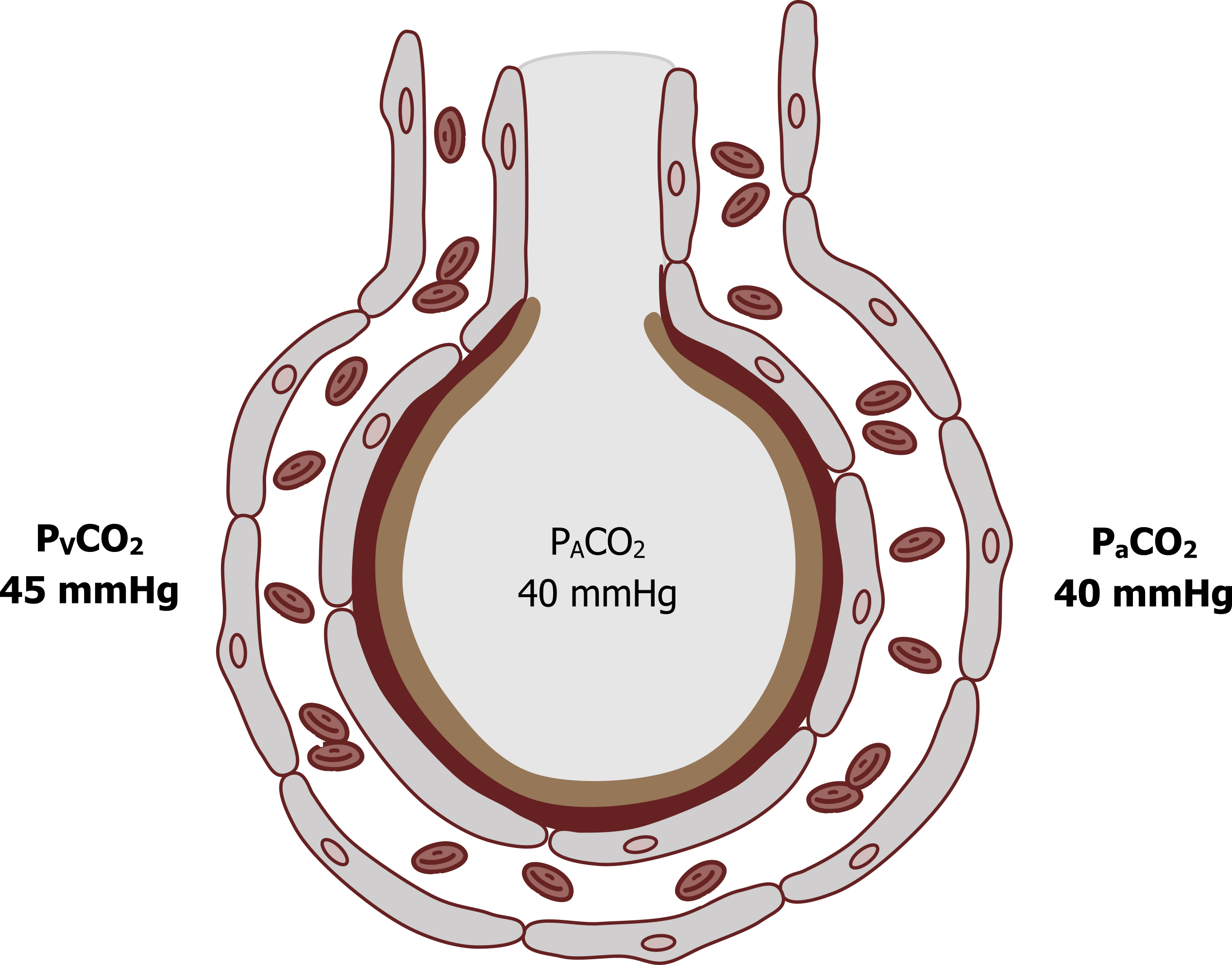
• Movement of carbon dioxide from pulmonary capillary blood to alveolar air
• Occurs across the respiratory membrane by diffusion
• Driven by partial pressure gradient between blood and alveoli
• Important for elimination of metabolic carbon dioxide
4
• Direction of diffusion
• Carbon dioxide diffuses from pulmonary capillary blood (higher PCO₂) to alveolar air (lower PCO₂).
• High solubility of CO₂
• Carbon dioxide is about 20 times more soluble than oxygen, so it diffuses very rapidly across the respiratory membrane.
• Small pressure gradient required
• Only a small pressure difference is needed:
• Pulmonary capillary PCO₂ ≈ 45 mmHg
• Alveolar PCO₂ ≈ 40 mmHg
• Efficiency of carbon dioxide removal
• Because of its high diffusibility, CO₂ elimination remains effective even if the respiratory membrane becomes slightly thickened.
This is a clever piece of evolutionary engineering. Carbon dioxide leaves the blood easily, even when the lungs are not working perfectly.
• Refers to blood flow through pulmonary capillaries surrounding alveoli
• Essential for effective gas exchange
• Must be properly matched with ventilation
4
• Definition of perfusion
• Perfusion refers to the flow of blood through pulmonary capillaries available for gas exchange.
• Importance in gas exchange
• Oxygen uptake and carbon dioxide removal require adequate blood flow around ventilated alveoli.
• Relationship with ventilation
• Efficient respiration depends on proper matching between ventilation (airflow) and perfusion (blood flow).
• Ventilation–perfusion ratio (V/Q ratio)
• The ratio between alveolar ventilation and pulmonary blood flow.
• Normal average V/Q ratio ≈ 0.8.
• Clinical importance
• Mismatch between ventilation and perfusion can lead to:
• Hypoxemia
• Pulmonary diseases such as embolism, COPD, and pneumonia
Get the full PDF version of this chapter.