Login
Welcome back! Please enter your details.
or
Don't have an account? Register here
Create Account
Join MedMentorEdu and start your medical journey.
or
Already have an account? Login here
Enhance your knowledge with our comprehensive guide and curated study materials.
4
• Definition of cardiovascular system
• The cardiovascular system, also known as the circulatory system, is the system responsible for transport of blood, nutrients, gases, hormones, and metabolic waste throughout the body.
• Components of the system
• Heart
• The heart is a muscular pumping organ that maintains blood circulation by rhythmic contraction.
• Blood vessels
• Blood vessels form a network of tubes through which blood circulates.
• These include arteries, arterioles, capillaries, venules, and veins.
• Blood
• Blood is the circulating fluid that transports oxygen, nutrients, hormones, and waste products between different tissues.
• Functions of cardiovascular system
• Transport of oxygen from lungs to tissues and carbon dioxide from tissues to lungs.
• Delivery of nutrients and hormones to body cells.
• Removal of metabolic waste products.
• Regulation of body temperature, pH, and fluid balance.
• Pulmonary circulation
• Pulmonary circulation refers to the movement of blood between the heart and lungs.
• Deoxygenated blood from the right ventricle travels to the lungs, where it becomes oxygenated and returns to the left atrium.
• Systemic circulation
• Systemic circulation involves transport of oxygenated blood from the left ventricle to all parts of the body.
• After delivering oxygen and nutrients, deoxygenated blood returns to the right atrium of the heart.
• Role in homeostasis
• The cardiovascular system helps maintain internal stability (homeostasis) by regulating blood pressure, temperature, electrolyte balance, and distribution of nutrients and oxygen.
• Clinical relevance
• Disorders of the cardiovascular system include hypertension, coronary artery disease, heart failure, and stroke, which can significantly affect body function and survival.
4
• Location of the heart in thoracic cavity
• The heart is located in the thoracic cavity between the lungs.
• It lies behind the sternum and above the diaphragm.
• Position in mediastinum
• The heart is situated in the middle mediastinum, a central compartment of the thoracic cavity.
• About two-thirds of the heart lies to the left of the midline and one-third to the right.
• Coverings of the heart (pericardium)
• The heart is enclosed within a double-walled sac called the pericardium.
• The pericardium consists of:
• Fibrous pericardium – outer tough protective layer.
• Serous pericardium – inner layer with parietal and visceral layers.
• The pericardial cavity between these layers contains pericardial fluid, reducing friction during heart movements.
• Chambers of the heart
• The heart contains four chambers that regulate blood flow.
• Right atrium
• Receives deoxygenated blood from the body through the superior and inferior vena cava.
• Right ventricle
• Pumps deoxygenated blood to the lungs through the pulmonary artery.
• Left atrium
• Receives oxygenated blood from the lungs through the pulmonary veins.
• Left ventricle
• Pumps oxygenated blood to the entire body through the aorta.
• Septa separating chambers
• The chambers are separated by muscular partitions called septa.
• Interatrial septum separates the atria.
• Interventricular septum separates the ventricles.
• Great vessels connected to heart
• Major blood vessels connected to the heart include:
• Superior vena cava
• Inferior vena cava
• Pulmonary artery
• Pulmonary veins
• Aorta.
• Blood flow pathway through heart
• Blood flows through the heart in the following sequence:
• Body → Right atrium → Right ventricle → Pulmonary artery → Lungs → Pulmonary veins → Left atrium → Left ventricle → Aorta → Body.
4
• Function of cardiac valves
• Cardiac valves ensure one-way flow of blood through the heart chambers.
• They open and close according to pressure differences between chambers and vessels.
• Their main function is to prevent backward flow of blood during the cardiac cycle.
• Atrioventricular valves
• Atrioventricular (AV) valves are located between the atria and ventricles.
• They allow blood to flow from atria to ventricles during ventricular filling.
• Tricuspid valve
• The tricuspid valve lies between the right atrium and right ventricle.
• It has three cusps (leaflets) and prevents backflow of blood into the right atrium during ventricular contraction.
• Mitral (bicuspid) valve
• The mitral valve is located between the left atrium and left ventricle.
• It has two cusps and prevents backflow of blood into the left atrium during ventricular systole.
• Semilunar valves
• Semilunar valves are located at the exits of the ventricles where blood leaves the heart.
• Pulmonary valve
• The pulmonary valve is present between the right ventricle and pulmonary artery.
• It prevents backflow of blood from the pulmonary artery into the right ventricle.
• Aortic valve
• The aortic valve lies between the left ventricle and the aorta.
• It prevents backflow of blood from the aorta into the left ventricle.
• Structure of valves
• Cardiac valves are composed of fibrous connective tissue covered by endocardium.
• Atrioventricular valves are supported by chordae tendineae and papillary muscles, which prevent valve prolapse during ventricular contraction.
• Prevention of backflow
• During ventricular contraction, the valves close tightly to prevent regurgitation of blood.
• This mechanism maintains efficient forward flow of blood through the circulatory system.
4
• Opening and closing during cardiac cycle
• Cardiac valves open and close rhythmically during the cardiac cycle.
• Their movement ensures that blood flows in the correct direction through the heart chambers and great vessels.
• Pressure differences controlling valve movement
• The opening and closing of valves are controlled by pressure differences between adjacent chambers and vessels.
• When pressure behind a valve exceeds the pressure ahead, the valve opens.
• When the pressure ahead becomes greater, the valve closes.
• Valve closure producing heart sounds
• Closure of the valves produces the normal heart sounds heard during auscultation.
• First heart sound (S1) occurs due to closure of atrioventricular valves (mitral and tricuspid).
• Second heart sound (S2) occurs due to closure of semilunar valves (aortic and pulmonary).
• Coordination with ventricular contraction
• During ventricular systole, the atrioventricular valves close and the semilunar valves open, allowing blood to be ejected from the ventricles.
• During ventricular diastole, the semilunar valves close and the atrioventricular valves open, allowing blood to fill the ventricles.
• Importance in maintaining unidirectional blood flow
• Proper functioning of the valves ensures unidirectional flow of blood through the heart and circulation.
• Valve dysfunction can lead to regurgitation or stenosis, impairing efficient cardiac function.
4
• Cardiac muscle fibre structure
• Cardiac muscle fibres are short, cylindrical cells that branch and interconnect with neighboring fibres.
• These interconnected cells form a network within the myocardium.
• Striated appearance
• Cardiac muscle shows alternating dark and light bands (striations) due to the regular arrangement of actin and myosin filaments within sarcomeres.
• Branching fibres
• Unlike skeletal muscle, cardiac muscle fibres branch and join with adjacent cells, allowing efficient spread of electrical impulses.
• Single central nucleus
• Each cardiac muscle cell usually contains one centrally located nucleus, though occasionally two nuclei may be present.
• Intercalated discs
• Adjacent cardiac muscle cells are connected by intercalated discs, which contain desmosomes, fascia adherens, and gap junctions.
• These structures provide mechanical strength and rapid electrical conduction between cells.
• Abundant mitochondria
• Cardiac muscle fibres contain large numbers of mitochondria, supplying the ATP required for continuous rhythmic contraction of the heart.
• Sarcomere organization
• Myofibrils in cardiac muscle are arranged in sarcomeres, which act as the functional units responsible for contraction.
4
• Small branches of arteries
• Arterioles are the small branches of arteries that lead to capillary networks.
• Thick smooth muscle layer
• The walls of arterioles contain a relatively thick layer of smooth muscle in the tunica media.
• This muscular layer allows active regulation of vessel diameter.
• Major resistance vessels
• Arterioles are known as the major resistance vessels of the circulatory system.
• Changes in their diameter significantly influence peripheral resistance to blood flow.
• Regulation of blood flow to tissues
• By constricting or dilating, arterioles regulate the amount of blood reaching different tissues according to metabolic needs.
• Role in blood pressure regulation
• Because they control peripheral vascular resistance, arterioles play a major role in maintaining and regulating systemic blood pressure.

4
• Smallest blood vessels
• Capillaries are the smallest blood vessels in the circulatory system.
• They connect arterioles to venules, forming an extensive capillary network within tissues.
• Single endothelial cell layer
• The wall of a capillary consists of a single layer of endothelial cells resting on a basement membrane.
• This thin structure facilitates efficient exchange of substances between blood and tissues.
• Site of exchange between blood and tissues
• Capillaries are the primary sites where exchange of oxygen, nutrients, carbon dioxide, and metabolic waste occurs between blood and body tissues.
• Types of capillaries
• Continuous capillaries
• These capillaries have a continuous endothelial lining with small intercellular clefts.
• They are found in muscles, skin, lungs, and the central nervous system.
• Fenestrated capillaries
• Fenestrated capillaries contain small pores (fenestrations) in the endothelial cells.
• These pores allow rapid exchange of fluids and small molecules.
• They are commonly found in kidneys, endocrine glands, and intestines.
• Sinusoidal capillaries
• Sinusoidal capillaries have large openings and discontinuous endothelial lining, allowing passage of larger molecules and cells.
• Diffusion and filtration functions
• Exchange across capillaries occurs mainly through diffusion, filtration, and osmosis.
• These processes maintain nutrient supply and waste removal in tissues.


4
• Specialized capillaries
• Sinusoids are a specialized type of capillary with unique structural features that allow extensive exchange between blood and surrounding tissues.
• Larger lumen and discontinuous endothelium
• They possess a large irregular lumen and discontinuous endothelial lining with wide gaps.
• The basement membrane may also be incomplete or absent.
• Slower blood flow
• Blood flow through sinusoids is slower compared to normal capillaries, allowing greater time for exchange of substances.
• Found in liver, spleen, bone marrow
• Sinusoids are commonly present in organs involved in filtration and blood cell production, such as the liver, spleen, and bone marrow.
• Facilitate exchange of large molecules
• Due to their large openings, sinusoids permit passage of large plasma proteins, cells, and other macromolecules between blood and tissues.
• This property is essential for functions like detoxification in the liver and blood cell formation in bone marrow.

4
• Structure of venous valves
• Venous valves are thin flap-like structures present inside many veins.
• They project into the lumen and usually occur as paired cusps.
• Formed by folds of endothelium
• These valves are formed by folds of the tunica intima (endothelial lining of the vein) reinforced by connective tissue.
• Prevent backflow of blood
• Venous valves allow blood to flow only toward the heart.
• When blood tends to flow backward, the valve cusps close and prevent regurgitation.
• Important in venous return
• Valves assist the return of blood to the heart, especially against gravity.
• They work together with skeletal muscle contraction (muscle pump) to facilitate venous return.
• More prominent in lower limb veins
• Venous valves are particularly well developed in veins of the lower limbs, where blood must travel upward toward the heart against gravity.

4
• Definition
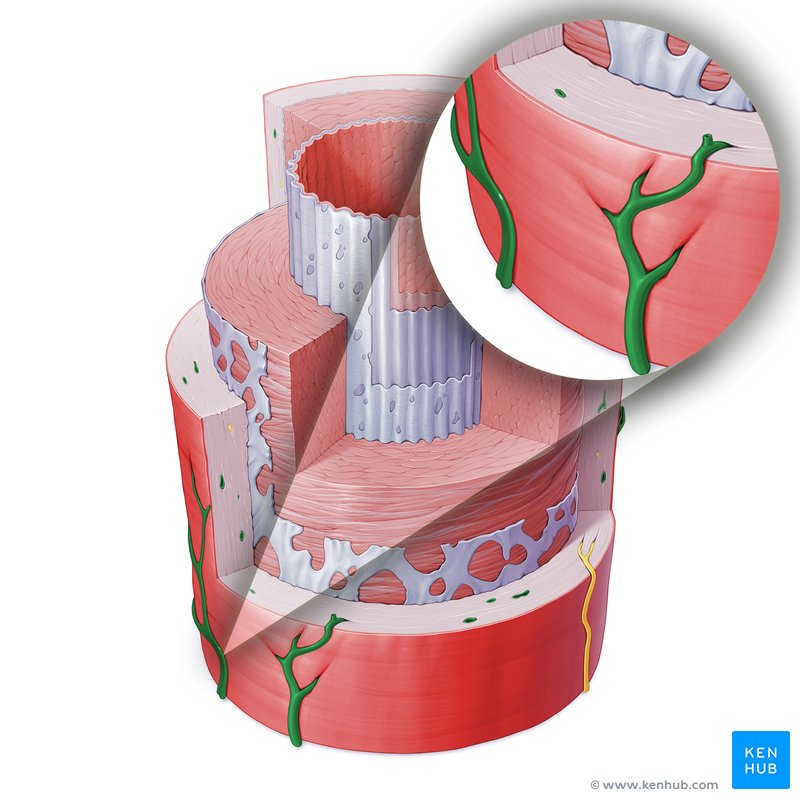
• Vasa vasorum are small blood vessels that supply the walls of large arteries and veins.
• Small vessels supplying large arteries and veins
• Large blood vessels have thick walls that cannot receive sufficient nutrients directly from the blood flowing through the lumen.
• Therefore, the vasa vasorum provide an additional blood supply to the vessel wall.
• Provide nutrients to vessel walls
• These vessels deliver oxygen and nutrients to the outer layers of the blood vessel wall and help remove metabolic waste.
• Located in outer layers of vessel
• Vasa vasorum are mainly located in the tunica adventitia and outer part of the tunica media of large arteries and veins.
• Important in large vessel physiology
• They play an important role in maintaining the health and function of large blood vessels.
• Damage or dysfunction of the vasa vasorum may contribute to vascular diseases such as atherosclerosis.
4
• Presence of lymphatic vessels in vessel walls
• Small lymphatic vessels are present in the outer layers of large blood vessels, particularly in the tunica adventitia.
• These lymphatics accompany the vasa vasorum and connective tissue surrounding the vessels.
• Drainage of excess fluid from vessel tissues
• Lymphatic vessels help remove excess interstitial fluid from the tissues of the vessel wall.
• This prevents fluid accumulation and maintains proper tissue environment.
• Role in immune defense
• Lymphatics transport immune cells such as lymphocytes and macrophages.
• They also carry antigens and foreign particles to lymph nodes, contributing to the body’s immune response.
• Maintenance of tissue fluid balance
• By draining excess interstitial fluid and returning it to the circulation, lymphatic vessels help maintain tissue fluid balance and normal vascular function.
4
• Specialized cardiac conduction system
• The heart contains a specialized system of modified cardiac muscle fibres known as junctional or conduction tissues.
• These tissues are responsible for generation and conduction of electrical impulses throughout the heart.
• Responsible for generation and conduction of impulses
• The conduction system produces spontaneous electrical impulses and transmits them rapidly through the myocardium.
• Coordinates rhythmic contraction of heart
• This system ensures coordinated contraction of atria and ventricles, allowing efficient pumping of blood.
• Components of conduction system
• The cardiac conduction system includes:
• Sinoatrial (SA) node
• Atrioventricular (AV) node
• Bundle of His
• Right and left bundle branches
• Purkinje fibres.

4
• Location in right atrium
• The SA node is located in the wall of the right atrium near the opening of the superior vena cava.
• Natural pacemaker of the heart
• The SA node is known as the natural pacemaker because it initiates electrical impulses that determine the heart rhythm.
• Generates spontaneous electrical impulses
• Cells of the SA node have the ability to generate impulses automatically without external stimulation.
• Sets heart rate
• The rate at which the SA node generates impulses determines the heart rate under normal conditions.
• Initiates cardiac cycle
• The electrical impulse produced by the SA node spreads through the atrial myocardium, initiating atrial contraction and the beginning of the cardiac cycle.
4
• Located in interatrial septum near AV junction
• The atrioventricular (AV) node is located in the lower part of the interatrial septum near the atrioventricular junction, close to the opening of the coronary sinus.
• Receives impulses from SA node
• Electrical impulses generated by the sinoatrial (SA) node travel through the atrial myocardium and reach the AV node.
• Delays conduction before ventricular activation
• The AV node introduces a short delay in impulse conduction before transmitting the signal to the ventricles.
• This delay allows sufficient time for the atria to contract and push blood into the ventricles.
• Ensures proper atrial contraction before ventricular contraction
• Because of this delay, atrial systole occurs before ventricular systole, ensuring efficient filling of the ventricles.
4
• Conducting pathway from AV node to ventricles
• The bundle of His, also called the atrioventricular bundle, is the pathway that conducts impulses from the AV node to the ventricles.
• Located in interventricular septum
• It passes from the AV node into the upper part of the interventricular septum.
• Divides into right and left bundle branches
• The bundle of His divides into right and left bundle branches, which run along the interventricular septum toward the apex of the heart.
• Transmits impulses rapidly to ventricular muscle
• These bundle branches conduct impulses to Purkinje fibres, which distribute the electrical signal throughout the ventricular myocardium, producing coordinated ventricular contraction.
4
• Terminal branches of cardiac conduction system
• Purkinje fibres are the terminal branches of the cardiac conduction system.
• They arise from the right and left bundle branches of the bundle of His.
• Spread impulses through ventricular myocardium
• These fibres extend throughout the ventricular walls and distribute electrical impulses to the ventricular muscle cells.
• Rapid conduction velocity
• Purkinje fibres conduct impulses very rapidly due to their large diameter and specialized structure.
• This allows the electrical signal to reach all parts of the ventricles almost simultaneously.
• Ensures coordinated ventricular contraction
• Because of rapid impulse transmission, both ventricles contract in a coordinated manner, enabling efficient ejection of blood into the pulmonary artery and aorta.
Get the full PDF version of this chapter.